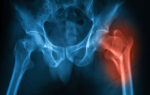
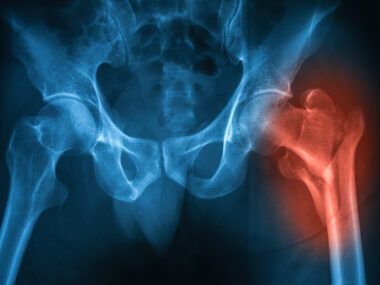
Hip surgery complications increase hospital stays, costs for AS patients
Post-surgery anemia and infections drove longer hospital stays, higher costs in US
Written by |
Ankylosing spondylitis (AS) patients undergoing total hip replacement face longer hospital stays and higher related costs than other patients after the surgery, according to an analysis of hospital records.
More complications, including anemia and infections, soon after surgery drove these increases in stays and admission-related costs, researchers noted.
These findings can be used to make informed decisions and implement strategies to improve patient outcomes and reduce healthcare costs.
The hospital records analysis was published in the Journal of Clinical Orthopaedics and Trauma, in the study “Ankylosing spondylitis substantially increases health-care costs and length of hospital stay following total hip arthroplasty – National in-patient database study.”
Arthritis of the hip affects 50% of AS patients
AS is a type of arthritis that mainly affects the joints of the spine but also those of the hips, shoulders, ribs, hands, and feet. Hip involvement affects about 50% of patients.
Many patients with AS-related hip damage require total hip replacement surgery, also called hip arthroplasty, which involves surgically removing damaged bone and cartilage, then replacing the hip with an artificial joint.
Studies suggest that AS patients undergoing hip replacement have an increased risk of complications around the time of surgery. However, information is lacking about how much it costs to care for these patients and what factors might complicate care.
Researchers used data from the Nationwide In-patient Sample (NIS), a large database of hospital records, to better understand the costs and challenges of taking care of patients diagnosed with AS who undergo hip replacement.
“Being the largest available data of hospital admissions, NIS database provides the ideal patient sample for evaluating such a complex problem,” the team wrote.
AS patients constituted 501 (0.14%) of the 367,890 patients who underwent hip replacement between 2016 and 2019. The remaining 367,389 (99.86%) cases were considered general population controls.
Compared with the controls, AS patients were significantly younger (mean 58.6 years vs. 65.9) and less likely to be female (32.9% vs. 55.9%). The two groups also had a different ethnicity distribution but similar rates of co-existing medical conditions (including diabetes and obesity) and hospital admissions following an emergency room visit. Specifically, the AS group had a significantly higher proportion of Asian patients than the control group.
Analysis revealed that people with AS had a longer hospital stay on average after hip replacement compared with other patients (2.5 vs. 2.3 days), with a higher total cost of care ($72,950 vs. $66,872). No differences were seen between groups in the type of facility they were transferred to after leaving the hospital.
Significantly higher risk of infections and anemia seen in AS patients
Overall, the complication rate was higher with AS patients than with controls. A significantly higher risk of developing infections related to the artificial joint (2.4% vs. 1.0%), a major complication of hip replacement surgery, occurred in AS patients. They also had significantly higher rates of anemia (21.8% vs. 11.8%) — a condition marked by low levels of healthy red blood cells.
The need for blood transfusion, the rate of pneumonia, and mortality were not statistically different between groups. Artificial joint fractures, dislocations, and mechanical complications were also similar.
The researchers then compared the two groups after matching individuals for pre-surgical factors, such as age, sex, obesity, diabetes, and tobacco use. Higher rates of anemia caused by blood loss were significantly higher in AS patients (21.76%) than in controls (15.89%). The most common local hip replacement complication in those with AS was an artificial joint-related infection (2.4% vs. 0.84%).
“Patients with AS require longer duration of hospital stay and higher admission-related expenditure following [total hip replacement surgery], in comparison with the general population,” the researchers concluded. “These enhanced early health care associated costs can be attributed to relatively higher complication rates in AS patients.”